Have you ever experienced stretches of time where you felt unstoppable — barely needing sleep, full of ideas, spending freely, taking risks — followed by periods where getting out of bed felt impossible?
This pattern of extreme highs and crushing lows is among the most recognizable signs of Bipolar Disorder — a mood condition affecting an estimated 2.8% of adults in the United States, and one of the most commonly misdiagnosed conditions in mental health.
This free online Bipolar Test is designed to help you explore whether your mood patterns align with the recognized criteria for bipolar disorder. It is not a diagnostic tool — only a licensed mental health professional can diagnose bipolar disorder, but it can give you meaningful insight and help you decide whether to seek a professional evaluation.
Your responses are completely private and anonymous. Results are instant.
What Is Bipolar Disorder?
Bipolar Disorder — formerly known as manic depression — is a mood disorder characterized by distinct episodes of mania or hypomania (extreme highs) alternating with episodes of depression (extreme lows). Between episodes, many people function well and feel like themselves.
Unlike everyday mood swings, bipolar episodes are intense, long-lasting, and represent a clear change from a person’s usual behavior. A manic episode can last days to weeks. A depressive episode can last weeks to months. The disorder is strongly influenced by genetics and brain chemistry — it is not caused by personal weakness or life circumstances alone.
Bipolar disorder is highly treatable. With the right combination of medication and therapy, the majority of people with bipolar disorder achieve good symptom control and lead full, stable lives.
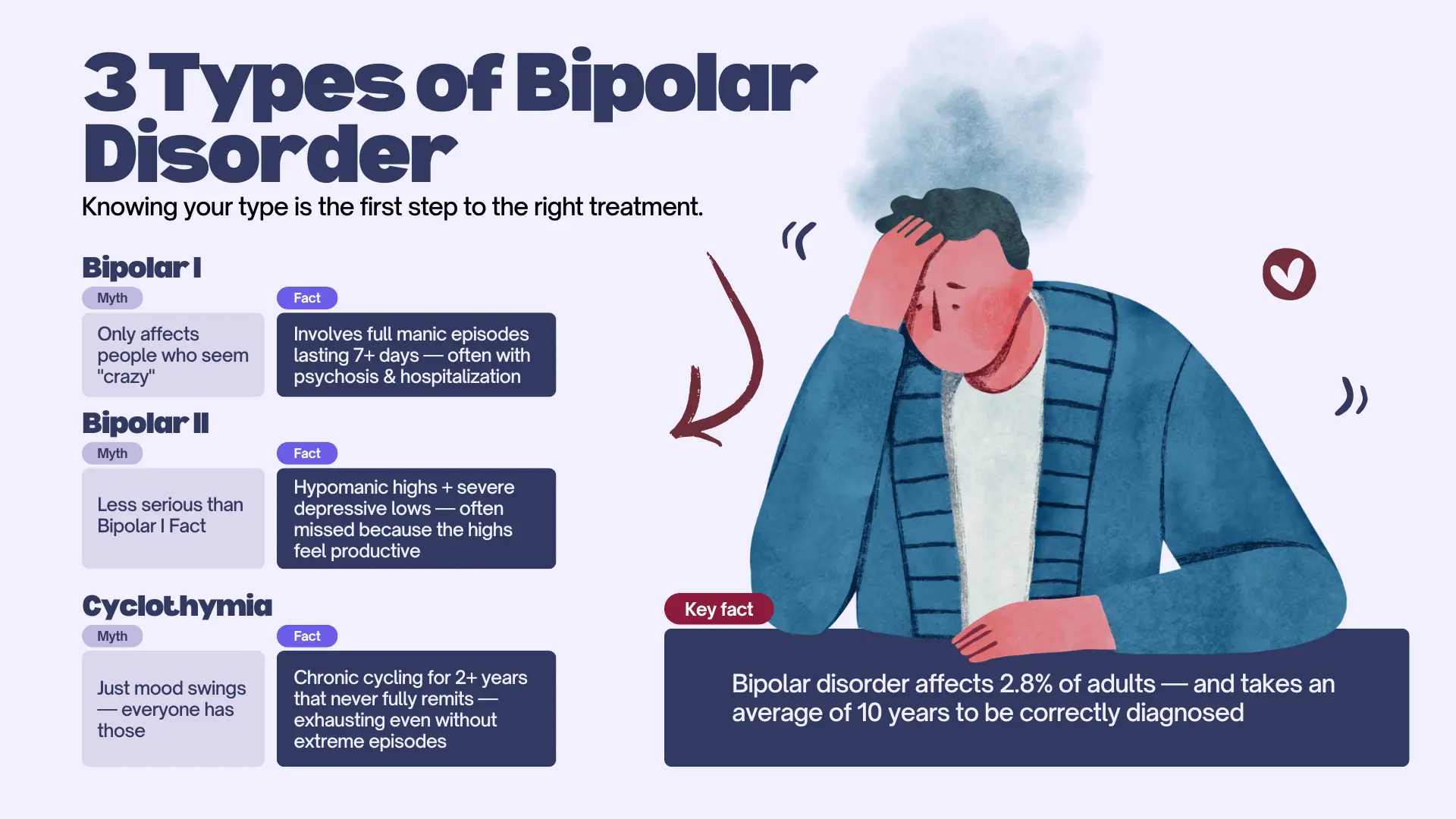
The 3 Types of Bipolar Disorder (DSM-5)
The DSM-5 recognizes three primary types of bipolar disorder. Understanding which type may apply to you is important, because they have different patterns and treatment approaches.
Bipolar I Disorder
Defined by at least one full manic episode lasting 7 days or more — or less if hospitalization is required. Depressive episodes are common but not required for diagnosis. Bipolar I mania can be severe enough to cause psychosis, risky behavior, and significant disruption to daily functioning.
Bipolar II Disorder
Defined by at least one hypomanic episode (a less intense form of mania, lasting at least 4 days) and at least one major depressive episode. Bipolar II is often missed because hypomania can feel productive and positive — people may not recognize it as a symptom. The depressive episodes in Bipolar II tend to be more frequent and debilitating than the highs.
Cyclothymic Disorder (Cyclothymia)
A milder but chronic form characterized by numerous periods of hypomanic symptoms and depressive symptoms over at least 2 years, without meeting the full criteria for a hypomanic or major depressive episode. Cyclothymia is often undiagnosed because neither the highs nor lows are severe enough to feel like a “real” disorder — but the instability is constant and exhausting.
Signs of a Manic Episode
A manic episode involves a distinct period of abnormally elevated, expansive, or irritable mood and increased goal-directed activity. Three or more of the following must be present to meet the DSM-5 criteria:
- Inflated self-esteem or grandiosity — feeling unusually powerful, special, or capable of anything
- Decreased need for sleep — feeling rested after only 2–3 hours, or not sleeping at all
- More talkative than usual — rapid speech that is difficult to interrupt
- Racing thoughts — ideas jumping rapidly from topic to topic
- Distractibility — attention easily pulled to irrelevant stimuli
- Increased goal-directed activity — taking on multiple projects, excessive productivity or socializing
- Impulsive, risky behavior — spending sprees, sexual indiscretions, reckless investments, substance use
Signs of a Depressive Episode in Bipolar Disorder
Bipolar depression shares many features with major depression but occurs in a person who also experiences manic or hypomanic episodes. Five or more of the following must be present for at least two weeks:
- Persistent low mood, emptiness, or hopelessness
- Loss of interest or pleasure in activities once enjoyed
- Significant weight changes or appetite disturbance
- Sleep disturbance — either insomnia or sleeping too much
- Slowed thinking, speech, or movement (or restlessness and agitation)
- Fatigue and loss of energy
- Feelings of worthlessness or excessive guilt
- Difficulty concentrating or making decisions
- Recurrent thoughts of death or suicide
How This Bipolar Test Works
This assessment covers the core mood patterns associated with both manic and depressive episodes. For each statement, select the response that most accurately reflects your experience — not a single bad day, but patterns you have noticed over time.
Scoring: Your answers generate a total score placed in one of three ranges:
- Low bipolar traits — Few patterns aligned with bipolar criteria
- Moderate bipolar traits — Some mood patterns worth exploring with a professional
- High bipolar traits — Significant alignment with bipolar criteria; professional evaluation is strongly recommended
This test is for informational purposes only. It is not a clinical diagnosis.
Understanding Your Results
If your score is low: Your mood patterns do not closely align with bipolar criteria. However, if you are experiencing distress, persistent low mood, or mood swings that affect your life, speaking with a professional is always worthwhile.
If your score is moderate: You may share some patterns with bipolar disorder, or these traits may reflect another condition such as ADHD, depression, anxiety, or BPD. Bipolar disorder is frequently misdiagnosed, and a full evaluation helps distinguish between them.
If your score is high: Your responses suggest significant alignment with bipolar disorder patterns. This does not confirm a diagnosis — only a clinical evaluation can do that — but it strongly suggests that speaking with a psychiatrist or mental health professional is the right next step. Bipolar disorder is treatable. Early and accurate diagnosis leads to better outcomes.
Bipolar Disorder vs Depression — A Critical Distinction
One of the most dangerous misdiagnoses in mental health is treating bipolar disorder as unipolar depression. Because people with bipolar disorder often seek help during depressive episodes — not manic ones — they are frequently prescribed antidepressants without a mood stabilizer, which can trigger manic episodes or worsen the overall course of the illness.
| Bipolar Disorder | Unipolar Depression | |
|---|---|---|
| Mood pattern | Highs and lows (episodic) | Lows only (no manic episodes) |
| Manic episodes | Present (defining feature) | Absent |
| Sleep during highs | Dramatically reduced need | Often increased (hypersomnia) |
| First-line treatment | Mood stabilizers + therapy | Antidepressants + therapy |
| Antidepressants alone | Can trigger mania — risky | Appropriate first-line option |
If you have ever experienced a period of time where you have unusually high energy, reduced sleep, or impulsive behavior alongside depression, it is important to tell your doctor — not just about the lows, but about the highs too.
Treatment for Bipolar Disorder
Bipolar disorder is a lifelong condition, but it is one of the most treatable mental health diagnoses. The goal of treatment is not just to manage individual episodes but to achieve long-term mood stability.
Mood Stabilizers (first-line medication)
Lithium remains the gold standard mood stabilizer with decades of evidence behind it. Valproate (Depakote) and lamotrigine are also commonly used. Mood stabilizers reduce the frequency and severity of both manic and depressive episodes.
Atypical Antipsychotics
Medications such as quetiapine, olanzapine, and aripiprazole are used for acute manic episodes and as maintenance therapy. Some are also approved specifically for bipolar depression.
Psychotherapy
Cognitive Behavioral Therapy (CBT) helps identify and change thought patterns that can trigger episodes. Interpersonal and Social Rhythm Therapy (IPSRT) focuses on stabilizing daily routines — sleep, meals, and activity — which directly influence mood stability in bipolar disorder.
Lifestyle management
Sleep regularity is one of the most powerful tools for managing bipolar disorder. Disrupted sleep is both a trigger and an early warning sign of episodes. Regular sleep schedules, avoiding alcohol, and stress management are all clinically supported as part of comprehensive treatment.
Bipolar Disorder and Co-occurring Conditions
Bipolar disorder frequently occurs alongside other conditions, which can complicate diagnosis and treatment:
- Anxiety disorders — Present in up to 50% of people with bipolar disorder
- ADHD — Shared features of impulsivity and distractibility make these difficult to distinguish; both can co-occur
- Substance use disorders — People with bipolar disorder have elevated rates of alcohol and drug use, often as self-medication
- BPD (Borderline Personality Disorder) — Both involve mood instability; see our BPD Test for comparison
- PTSD — Trauma history is common and can worsen the course of bipolar disorder
Frequently Asked Questions About Bipolar Disorder
What is the difference between Bipolar I and Bipolar II?
Bipolar I requires at least one full manic episode — a severe, distinct period of elevated or irritable mood lasting at least 7 days, which can include psychosis and often requires hospitalization. Bipolar II involves hypomania — a milder, shorter elevated mood state — alongside major depressive episodes. Bipolar II is often missed because the hypomanic episodes can feel productive rather than problematic, and people typically seek help during the depressive phases.
Can bipolar disorder be mistaken for depression?
Yes — this is one of the most common misdiagnoses. Because people with bipolar disorder often present for help during depressive episodes, and may not recognize or report their hypomanic episodes, they are frequently diagnosed with depression and given antidepressants alone. Antidepressants without a mood stabilizer can trigger mania in people with bipolar disorder. This is why it is critical to tell your doctor about any periods of elevated mood, reduced sleep, or increased energy — not just the depressive episodes.
Is bipolar disorder genetic?
Yes — bipolar disorder has one of the strongest genetic influences of any mental health condition. Having a first-degree relative with bipolar disorder increases your risk significantly. Twin studies suggest heritability of around 80%. However, genetics alone do not determine outcome — environmental factors, stress, and sleep patterns all play important roles in whether and when episodes occur.
What does a manic episode feel like?
People in a manic episode often describe feeling extraordinarily capable, energetic, and clear-headed — at least initially. Ideas flow rapidly. Sleep feels unnecessary. There is a sense of importance or special purpose. However, manic episodes also bring impaired judgment, risky decisions, irritability, and — in severe cases — paranoia or psychosis. Many people with bipolar disorder only recognize a manic episode in hindsight, after the consequences become clear.
What is hypomania?
Hypomania is a less severe form of mania that does not cause the psychosis or extreme impairment of a full manic episode. People in a hypomanic state may feel unusually productive, sociable, and confident — which is why it often goes unrecognized or is even welcomed. However, hypomania is still a symptom of bipolar disorder (specifically Bipolar II) and tends to precede or follow depressive episodes. Without treatment, hypomanic episodes often escalate or cycle into depression.
Can bipolar disorder be treated without medication?
For most people, medication is an important part of managing bipolar disorder — particularly mood stabilizers for preventing recurrence of episodes. Therapy alone is generally not sufficient as a standalone treatment for moderate to severe bipolar disorder, though it is a crucial component alongside medication. Lifestyle factors — especially sleep regularity — have strong evidence supporting their role in mood stability and can complement medication significantly.
How is bipolar disorder diagnosed?
Bipolar disorder is diagnosed by a psychiatrist or mental health professional through a structured clinical interview, typically using DSM-5 criteria. Screening tools such as the Mood Disorder Questionnaire (MDQ) — developed by Dr. Robert Hirschfeld — are commonly used as a first step. A thorough evaluation also rules out medical causes of mood symptoms such as thyroid disorders. Online tests like this one are screening tools only — a starting point for reflection, not a diagnosis.
Related Tests
- Bipolar Depression Test — explore the depressive side of bipolar disorder specifically
- Cyclothymia Test — screen for the milder, chronic form of bipolar spectrum disorder
- BPD Test — compare bipolar mood patterns with borderline personality disorder
- Depression Test — if you only experience lows with no elevated episodes
- Anhedonia Test — loss of pleasure is common in both bipolar depression and major depression
- Intermittent Explosive Disorder Test — irritability and impulsivity overlap with manic episodes
The postpartum period carries a particularly elevated risk of mood episodes for women with bipolar disorder — if you are pregnant or recently gave birth, the EPDS should be completed alongside this screening.
References
- American Psychiatric Association. (2022). Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition, Text Revision (DSM-5-TR). Washington, DC: APA. psychiatry.org
- Hirschfeld, R. M. A., et al. (2000). Development and validation of a screening instrument for bipolar spectrum disorder: The Mood Disorder Questionnaire. American Journal of Psychiatry, 157(11), 1873–1875. doi:10.1176/appi.ajp.157.11.1873
- National Institute of Mental Health. (2023). Bipolar Disorder. nimh.nih.gov
- Merikangas, K. R., et al. (2011). Prevalence and correlates of bipolar spectrum disorder in the World Mental Health Survey Initiative. Archives of General Psychiatry, 68(3), 241–251. doi:10.1001/archgenpsychiatry.2011.12
- Vieta, E., et al. (2018). Bipolar disorders. Nature Reviews Disease Primers, 4, 18008. doi:10.1038/nrdp.2018.8


